2018/19 Update: This has been one of my most popular articles over the years, and the data for DHEA...
23 search results for: dhea
Contact Me contact@brinkzone.com
DHEA – does it have any beneficial non-hormonal effects?
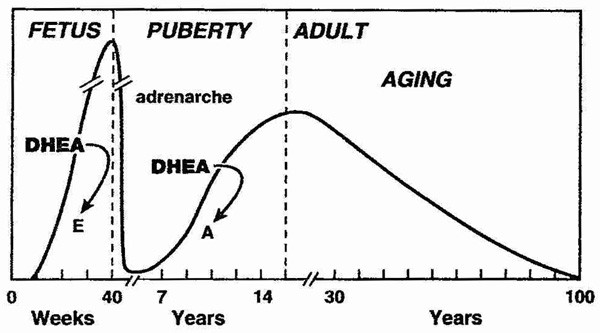
DHEA (dehydroepiandrosterone) is most known for being a pro-hormone which in the body gets converted to testosterone and estrogen....
DHEA supplementation in older adults – good or bad?
Will has previously mentioned DHEA as it relates to hormonal effects and health promotion: http://www.brinkzone.com/general-health/dhea-hormone-facts http://www.brinkzone.com/articles/dhea-the-most-underrated-supplement-for-women http://www.brinkzone.com/articles/xv-international-symposium-on-atherosclerosis When it...
Below is a brief discussion on DHEA as “muscle builder” and such. DHEA may have specific benefits to women,...
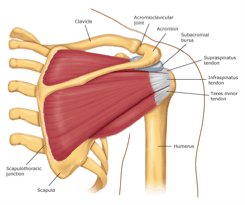
A Common Cause of Pain For Fitness Oriented People And Athletes Alike Tennis elbow or Lateral epicondylitis is inflammation,...
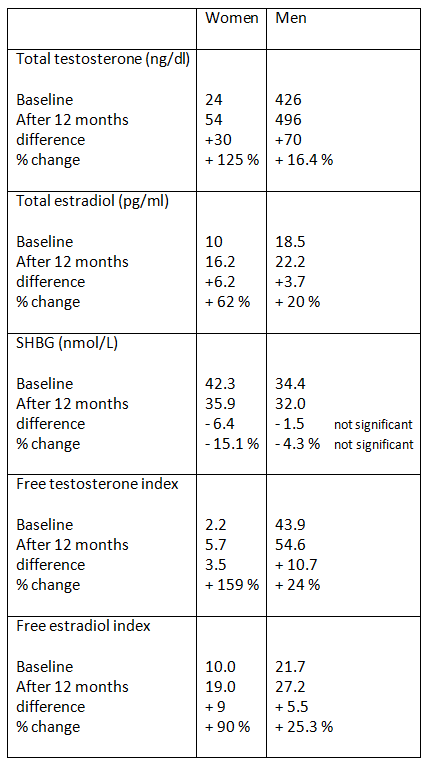
Testosterone In WOMEN – is it physiological and clinically important?
EDITORS NOTE: A recent video I (Will Brink) did HERE also discusses the fact T is just as important...
How many times have we done or seen people at the gym doing the “wind-mill” stretch before a workout? ...
Combined Testosterone and GH therapy for best results on body composition and safety profiles
Many studies have highlighted the importance of investigating all major hormones, and correcting deficiencies and imbalances if present. Given...
"Fish Oil," Friend or Foe To The Prostate?
Another great article from Dr. Lopez that examines in objective detail what risks, if any, long chain fatty acids...
Omega-3 Madness: Clarifying Recent Research
Note From Will: Folks, I didn’t write this article. Dr. Lopez did. It’s an excellent review of the recent...