A pervasive dieting mantra is that a cumulative reduction of caloric intake of 3,500 will result in a weight...
Author Archive for: Monica
Contact Me contact@brinkzone.com
To most people, the mere word “muscles” brings to mind huge muscular bodybuilders. The importance of muscle mass, strength,...
How to get most out of your Creatine – what form, dose and supplementation strategy?
Creatine is one of the few dietary supplements that have a very solid scientific support for its efficacy in...
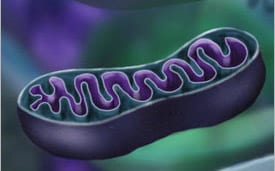
Exercise Mimetics & Mitochondrial Boosters
Mitochondria are the ‘energy powerhouse of the cell’ that convert the foods we eat to usable energy our body...
Testosterone deficiency and treatment is a very misunderstood and controversial topic among scientists, regulatory agencies (such as the FDA...
January 7th 2016, the new 2015 Dietary Guidelines for Americans were released: http://health.gov/dietaryguidelines/2015/guidelines/ One would expect this to be a...
Krill oil is becoming increasingly popular, and many people use it as an alternative to fish oil, since both...
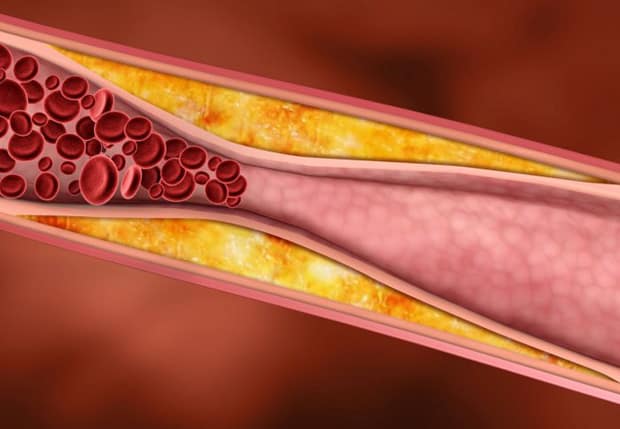
Why you need to look beyond your LDL – “bad cholesterol” – level
In the United States, cardiovascular diseases account for about 1 of every 3 deaths. The cornerstone in heart disease...
Effects of Testosterone Administration for 3 Years on Subclinical Atherosclerosis Progression in Older Men
Clinical practice guidelines rely heavily on results from randomized controlled trials (RCTs), which is the gold standard for medical...
Long-term testosterone treatment with different testosterone preparations – provocative results on diagnosis and adherence
Due to lack of consistent clear-cut guidelines for diagnosis and treatment of testosterone deficiency, there is a lot of...
BrinkZone Authors
Categories
Recent Posts
- Oreo Cookies Better Than Statins For lowering LDL?! March 12, 2024
- Oreo Cookies Vs Statins?! March 7, 2024
- Lactoferrin: A Broad Spectrum Anti-Viral January 25, 2024
- Pragmatic Real World *Permanent* Weight Loss! November 10, 2023
- Psychology 101 Of Weight Loss November 2, 2023
- Creatine in Post-Viral Fatigue Syndrome/Long Covid October 4, 2023
- Iron, The Key To Glucose Metabolism And Disease Prevention? September 27, 2023
- NAC Vs Gly-NAC Vs Glyteine Vs Whey! August 24, 2023









Recent Comments